 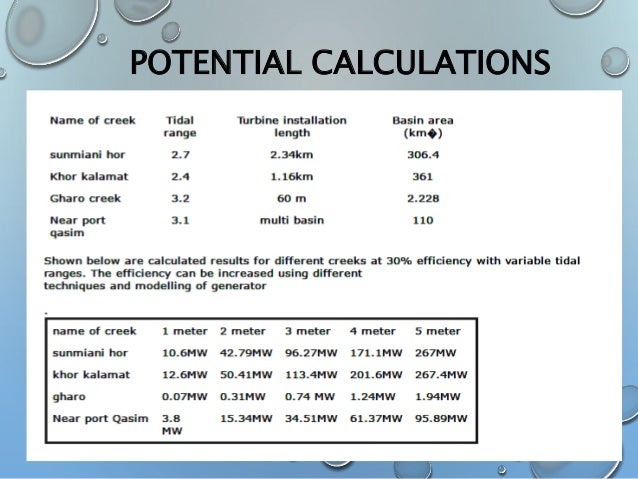
One dataset allowed median weight to be directly related to height over the 45–110 cm range, the weight-for-recumbent length standard compiled by the World Health Organization (WHO). Instead, ‘lean’ body weight was assumed to be adequately represented by median weight during growth across healthy populations. The literature search did not divulge this ‘ideal’ data set. Publications were reviewed primarily from the viewpoint of protective ventilation, rather than pharmacokinetics or other applications of weight estimation.Īn ideal data set for this feasibility analysis would have been known lean body weights for all statures across a broad population. 
Search terms were: protective ventilation, predicted body weight, ideal body weight, pediatric ventilation, growth charts, and related terms. Relevant clinical and biomedical engineering literature were identified by searching PubMed (up to June 2016). This analysis determined whether it was feasible for body-weight predictive formulae to be unisex and to span all body sizes (from infants to adults), while retaining adequate relevance to the outcomes of the landmark ARDSNet protective ventilation study. A unisex formula may simplify the task of applying lung-protective ventilation, and simplification may reduce error rates. Finally, the most established PBW formula includes the patient’s sex in addition to height, but it is unclear whether this is justified, particularly given the inaccuracies elsewhere in the process. For instance, growth charts may be required to estimate an ideal/predicted body weight from an estimated height/length (or surrogate). Recent publications have emphasized the challenge and complexity of extending protective ventilation into pediatrics. Meanwhile, for pediatric ventilation, there is no simple formula to estimate PBW: the dominant PBW formula (used in the ARDS Network trial and generally attributed to Devine ) is formally defined only for heights above about 5 ft/152 cm. Consequently standardization has been proposed. The difference in estimated PBW between these 2 approaches can vary by up to 30%. For adults, PBW formulae do exist, with 2 different approaches used to predict lean body mass in the early ARDS studies. 
There is the challenge of appropriately estimating a weight from the estimated height. If height cannot be measured or provided by the patient, more convenient surrogate measures such as arm-span, arm demispan, ulna length, or knee height have been devised. There is the challenge of obtaining a reasonable estimation of height (an issue not limited to protective ventilation alone). Such initiatives may be hindered by the multiple challenges in predicting weight from height. Various initiatives have been suggested to improve adherence, such as to change routine charting practices from the absolute tidal volumes (mL) to mL/kg PBW, or to configure alarms around mL/kg PBW rather than absolute volumes. ĭespite consensus in favor of lung protective ventilation, multiple surveys suggest that adherence is not uniform, with much scope for improvement. The tidal volume scaling factor is 5–8 mL/kg of predicted body weight (PBW) (or less at elevated plateau pressure). 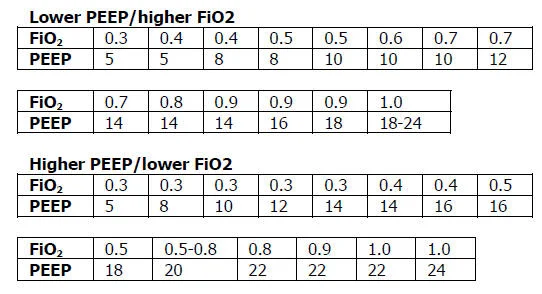
Therefore, by calculating initial tidal volume based on predicted (or lean) body weight rather than actual weight, configuration of the ventilator retains some connection to metabolic need (weight), while also reducing potential for volutrauma (height). Lung capacity and respiratory system compliance relate more closely to height than to weight, at least in normal subjects. The use of predicted weight is based on the assumption that volutrauma might be minimized by delivering a volume appropriate to the patient’s lung capacity. Key elements of a lung-protective strategy are the application of positive end-expiratory pressure (PEEP), limitation of plateau pressure, and a minimal tidal volume scaled to a ‘predicted’, rather than actual, body weight. Recent consensus guidance recommends the lung-protective strategy also be applied in pediatric acute lung injury. Lung-protective ventilation has also been shown to improve outcomes in patients ventilated in the operating room and in the intensive care unit (ICU). However, a ‘lung-protective strategy’ is increasingly the standard of care for acute ventilation based on data showing that this approach to treating acute respiratory distress syndrome (ARDS) in adults was associated with reduced mortality. This remains common practice for pediatric ventilation, and for much of adult ventilation. Historically, mechanical ventilation was initiated with a tidal volume based on a patient’s actual body weight, which was believed to reflect metabolic need. 
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
